Neonatal mortality
Neonatal mortality, deaths in children within 28 days of birth, encompasses the effect of socio-economic and environmental factors on new-borns and mothers, and also the capacities and responsiveness of national health systems.
Prematurity, birth asphyxia and birth trauma and sepsis and other infectious conditions are the leading causes of deaths in newborns (WHO Health Observatory Data Repository). In Pakistan, these three causes accounted for 32.5 deaths per 1,000 live births in 2017. Mortality rates due to neonatal infections, birth asphyxia and birth trauma and prematurity steadily decreased since 2010 in all countries, except a slight increase reported in Fiji for mortality due to prematurity and infections and in Lao PDR for mortality due to infections. Congenital anomalies and other conditions arising during pregnancy are also listed as primary causes of mortality during the first four weeks of life. Undernutrition continues to be among the leading causes of death in both mothers and newborns [see sections “Young child malnutrition (including undernutrition and overweight)” and “Overweight and obesity” in Chapter 4]. In the Asia-Pacific region, around two-thirds of the deaths in the first year of life occur during the neonatal period.
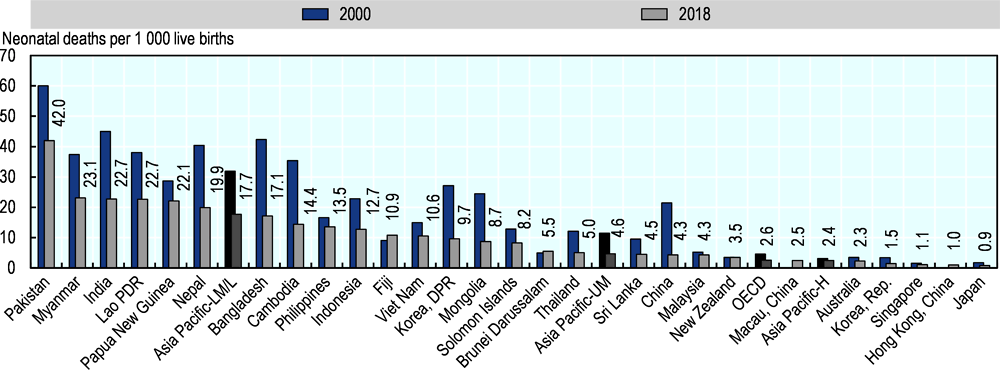
Sustainable Developing Goals set a target of reducing neonatal mortality to 12 deaths or less per 1 000 live births by 2030. In 2018, the average among lower-middle and low income countries in Asia-Pacific was 17.7 deaths per 1 000 live births, around half the rate observed in 2000 but still above the SDG target (Figure 3.4). Upper-middle income Asia-Pacific countries already reached the SDG target in 2000 reporting a rate – on average – of 11.5 deaths per 1 000 live births, which then decreased to 4.6 in 2018. High income countries reported neonatal mortality rates similar to those of the OECD, with an average of 2.4 deaths per 1 000 live births.
Geographically, countries in South and South-East Asia experienced higher neonatal mortality rates than those in eastern Asia and Australasia. Japan; Hong Kong, China; Singapore; the Republic of Korea and Australia reported two deaths or less per 1 000 live births in 2018, whereas neonatal mortality rates were higher than 20 in Papua New Guinea, the Lao PDR; India and Myanmar, and higher than 40 in Pakistan.
Between 2000 and 2018, the neonatal mortality rate has fallen in almost all Asia-Pacific countries (Figure 3.4). The rate in 2018 was one-third of the rate in 2010 in Korea DPR and Mongolia, while in China the rate reported in 2018 was one-fifth of the one reported in 2010. Both Brunei Darussalam and Fiji reported an increase in neonatal mortality rates during the period in this study.
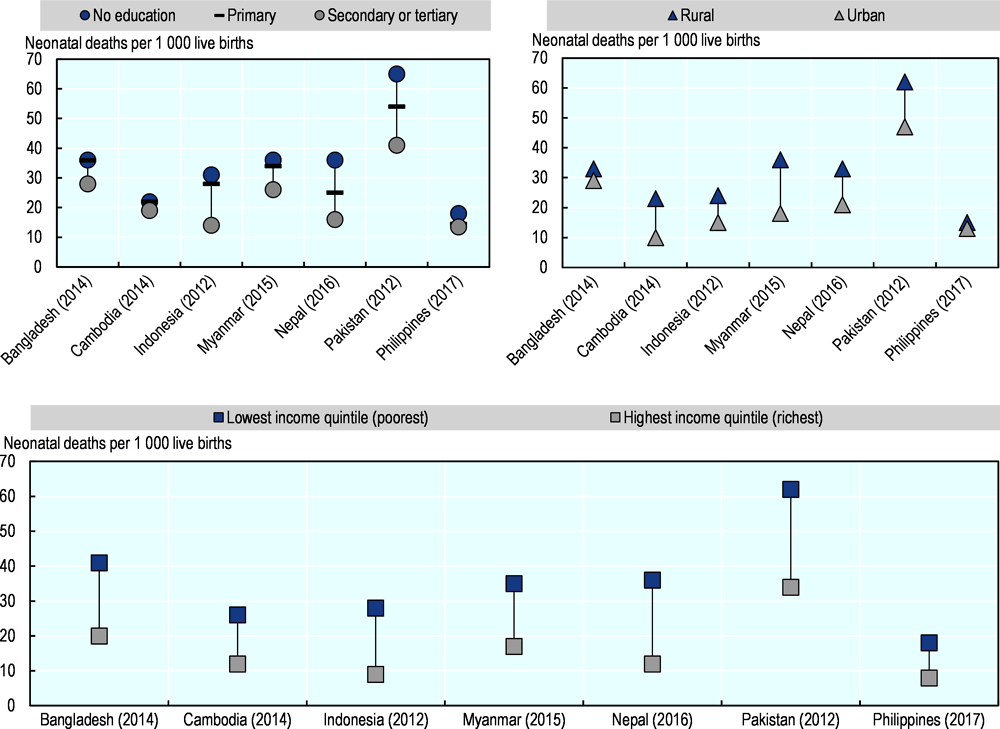
Key determinants of neonatal mortality rates across countries include income status, geographical location and mother education. For instance, in Indonesia and Nepal, neonatal mortality is three times or more higher in the poorest households compared to richest ones, and twice as high when mothers have no education rather than secondary or tertiary education. Geographical location is another determinant of differences reported in neonatal mortality in the region, though relatively less important in comparison to households’ income. For example, neonatal mortality rate in rural areas of Myanmar and Cambodia was twice the rate reported for urban areas (Figure 3.5).
Neonatal mortality rates recede through cost-effective and appropriate interventions. These include immediate skin-to-skin contact between mothers and newborns after delivery, and kangaroo mother care for babies weighing 2000g or less as well as neonatal resuscitation training, prevention and management of neonatal sepsis, reducing mortality from prematurity and low birthweight, and prioritizing the roles of breastfeeding and antenatal corticosteroids (Conroy, Morrissey and Wolman, 2014[4]).
Reductions in neonatal mortality will require not only providing quality care through the aforementioned strategies and systems strengthening, but also ensuring that all segments of the population benefit from quality care (Gordillo-Tobar, Quinlan-Davidson and Lantei Mills, 2017[5]).