Long-term care workers
Long-term care (LTC) is a labour-intensive service. Formal LTC workers are defined as paid staff, typically nurses and personal carers, providing care and/or assistance to people limited in their daily activities at home or in institutions, excluding hospitals. Formal care is complemented by informal, usually unpaid, support from family and friends, which accounts for a large part of care for older people in all OECD countries (see indicator on “Informal carers”).
Relative to the population aged 65 and over, Norway, Sweden and the United States have the most LTC workers and the Slovak Republic and Portugal the fewest (Figure 11.19). In all countries except for Israel, Japan, Estonia and Korea, the majority of LTC staff work in institutions, even though the majority of recipients usually receive care at home (see indicator on care recipients). This reflects the fact that those in institutions often have more severe needs and require more intensive care.
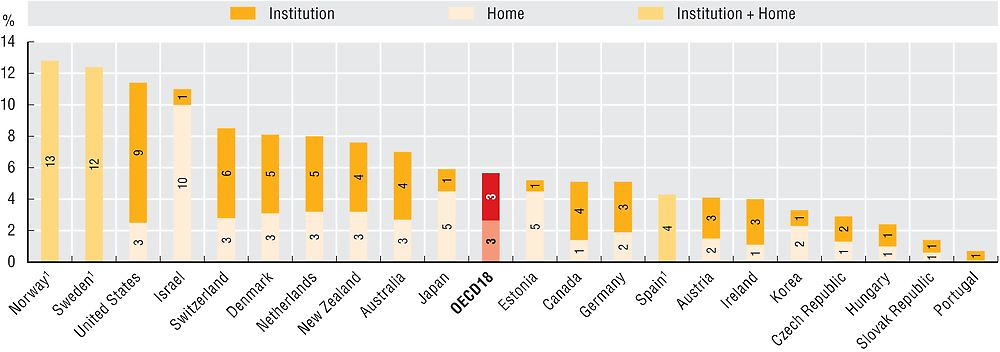
1. In Norway, Sweden and Spain it is not possible to distinguish LTC workers in institutions and at home. They are not included in the OECD average.
Source: OECD Health Statistics 2017.
Most LTC workers are women and work part-time. At least 90% of LTC workers are women in Korea, Denmark, the Slovak Republic, the Netherlands and Norway (Figure 11.20). Foreign-born workers also play an important role in LTC provision, though their presence is uneven across OECD countries. While Germany has very few foreign-born LTC workers, nearly one in four care workers in the United States is foreign-born (Colombo et al., 2011).
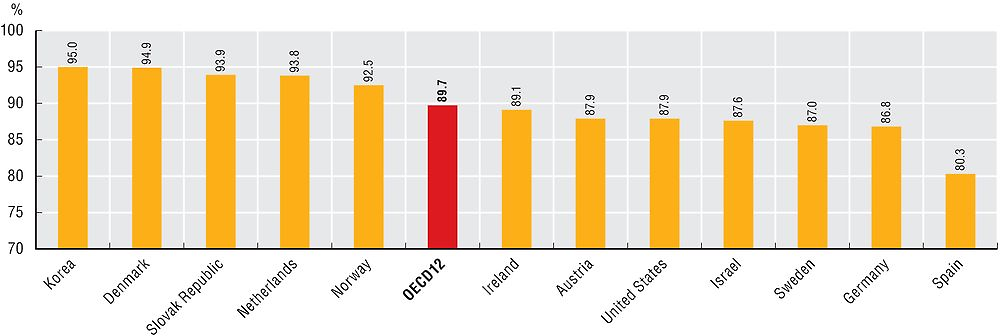
Source: OECD Health Statistics 2017.
The LTC sector represents a small but growing share of total employment in OECD countries, averaging just over 2%. The number of LTC workers increased by more than 50% in Japan, Korea, and Israel between 2005 and 2015 (Figure 11.21). In Japan and Korea, this is related to the introduction of universal LTC insurance and the increasing professionalisation of LTC work. However, the Japanese and Korean populations are ageing rapidly and even with these changes, the growth in the LTC workforce has only just kept pace with the growth in the population aged over 80 – the people most likely to need LTC. In contrast, the number of long-term care workers decreased in Estonia, the Slovak Republic, and the Netherlands, despite large increases in the population aged 80+ over the same period (Figure 11.21).
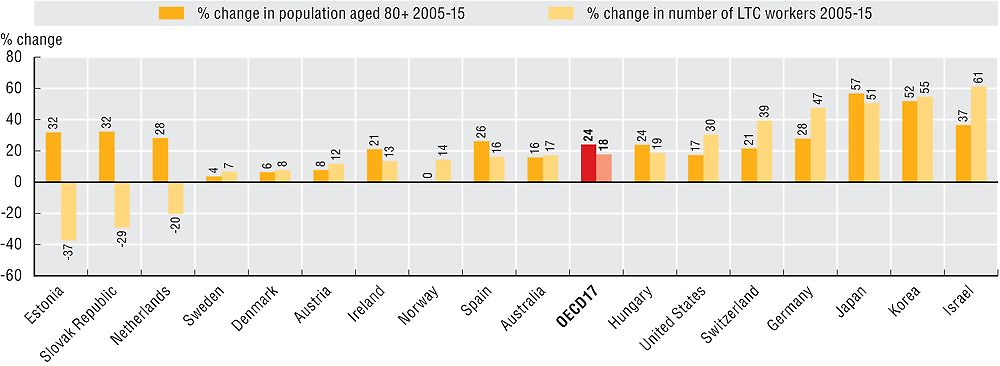
Source: OECD Health Statistics 2017.
On average, around one third LTC workers are nurses and the other two thirds are personal care workers (also referred to as nursing aides, health assistants in institutions or home-based care assistants) with less formal training. Many OECD countries have set educational and training requirements for personal care workers, although these vary substantially, especially where home-based care is concerned (OECD/European Commission, 2013).
As populations continue to age, demand for LTC workers is likely to rise. Responding to increasing demand will require policies to improve recruitment (e.g. encouraging more unemployed people to consider training and working in the LTC sector); improve retention (e.g. enhancing pay and work conditions); and increase productivity (e.g. through reorganisation of work processes and more effective use of new technologies) (Colombo et al., 2011; European Commission, 2013).
Long-term care workers are defined as paid workers who provide care at home or in institutions (outside hospitals). They include qualified nurses and personal care workers providing assistance with ADL and other personal support. Personal care workers include different categories of workers who may be called under different names in different countries. They may have some recognised qualification or not. Because personal care workers may not be part of recognised occupations, it is more difficult to collect comparable data for this category of LTC workers across countries. LTC workers also include family members or friends who are employed under a formal contract either by the care recipient, an agency, or public and private care service companies. They exclude nurses working in administration. The numbers are expressed as head counts, not full-time equivalent.
There are some differences in the methodologies that countries use to calculate the data, which could bias the results. Data for some countries refers only to workers employed in the public sector, while other countries include the private and non-profit sectors. Data from the Czech Republic and Japan are based on surveys of establishments, meaning that people who work in more than one establishment are double-counted.
References
Colombo, F. et al. (2011), Help Wanted? Providing and Paying for Long-Term Care, OECD Publishing, Paris, https://doi.org/10.1787/9789264097759-en.
OECD and European Commission (2013), A Good Life in Old Age? Monitoring and Improving Quality in Long-Term Care, OECD Health Policy Studies, OECD Publishing, Paris, https://doi.org/10.1787/9789264194564-en.
Scheil-Adlung, X. (2015), “Long-term Care (LTC) Protection for Older Persons: A Review of Coverage Deficits in 46 Countries”, ESS Working Paper, No. 50, International Labour Office, Geneva.
United Nations (2016), “The Growing Need for Long-term Care, Assumptions and Realities”, Briefing Paper.
