Consultations with doctors
Consultations with doctors can take place in doctors’ offices or clinics, in hospital outpatient departments or, in some cases, in patients’ own homes. In many European countries (e.g., Denmark, Italy, Netherlands, Norway, Portugal, Slovak Republic, Spain and the United Kingdom), patients are required or even incentivised to first consult a general practitioner (GP) about any new episode of illness. The GP may then refer them on to a specialist, if indicated. In other countries, patients may approach specialists directly.
In 2015, the number of doctor consultations per person ranged from less than 3 in Mexico and Sweden, to almost 13 and 16 in Japan and Korea respectively (Figure 9.1). The OECD average was 6.9 consultations per person per year, with most countries reporting between four and eight consultations. Cultural factors can play a role in explaining some of the variations across countries, although certain health system characteristics may also be important. Provider payment methods and the level of co-payments are particularly relevant. For example, some countries where doctors are paid on a fee-for-service basis tend to have above-average consultation rates (e.g. Japan and Korea), while countries with mostly salaried doctors tend to have below-average rates (e.g. Mexico, Finland and Sweden). However, there are examples of countries such as Switzerland and the United States where doctors are paid mainly by fee-for-service and where consultation rates are below average. In these countries, patient co-payments can be high, which may result in patients not consulting a doctor because of the cost of care (see the indicator on “Unmet needs for health care due to cost” in Chapter 5).
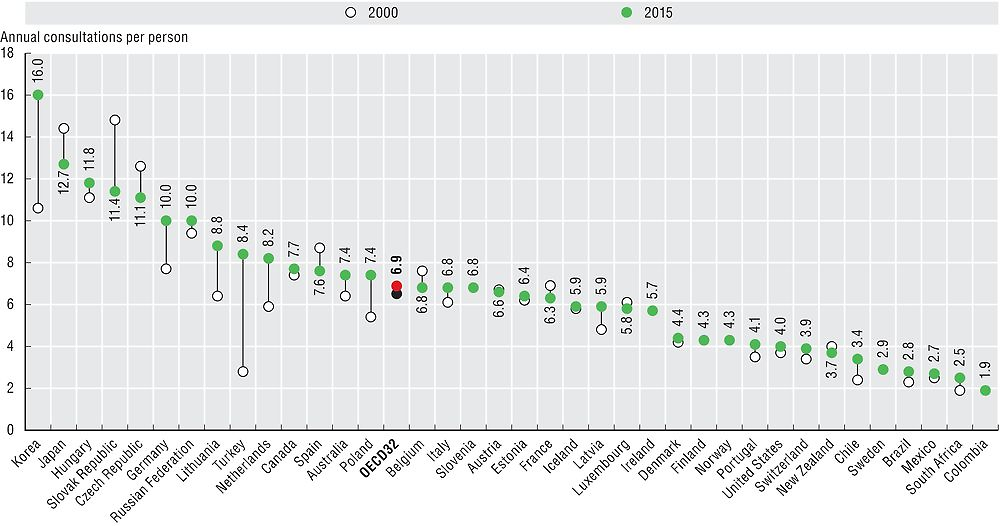
Source: OECD Health Statistics 2017.
In Sweden and Finland, the low number of doctor consultations may also be explained partly by the fact that nurses and other health professionals play a more important role in providing primary care to patients in health centres, lessening the need for consultations with doctors (Delamaire and Lafortune, 2010).
The average number of doctor consultations per person across the OECD has remained relatively stable since 2000 (from 6.5 to 6.9). But in some countries there have been large increases over time (Korea, Turkey). In some other countries, the number of doctor consultations per person fell. This was the case in Japan, the Czech Republic and the Slovak Republic, although the numbers remains well above average in these three countries.
Information on the number of doctor consultations per person can be used to estimate the annual numbers of consultations per doctor. This indicator should not be taken as a measure of doctors’ productivity, since consultations can vary in length and effectiveness, and because it excludes the services doctors might deliver for hospital inpatients, as well as on administration and research. Keeping this in mind, the estimated number of consultations per doctor is highest in Korea and Japan, followed by Turkey and Hungary (Figure 9.2). On the other hand, the estimated number of consultations per doctor was lowest in Sweden and Norway, where consultations with doctors in both primary care and hospital settings tend to be focused towards patients with more severe and complex cases.
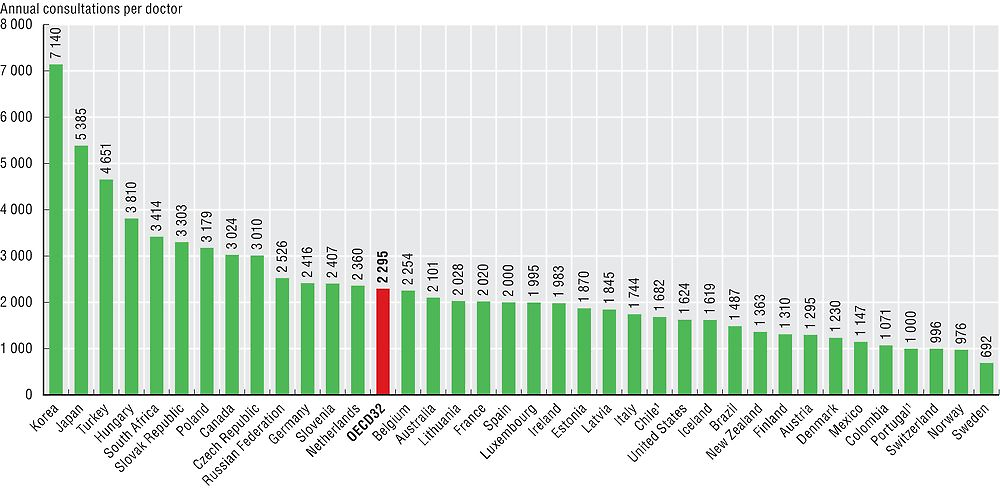
1. In Chile and Portugal, data for the denominator include all doctors licensed to practice.
Source: OECD Health Statistics 2017.
The number and type of doctor consultations can vary among different socio-economic groups in each country. An OECD study found that the probability of a visit to the GP tends to be equally distributed in most countries, but in nearly all countries, higher income people are more likely to see a specialist than those with low income, and also more frequently (Devaux and de Looper, 2012).
Consultations with doctors refer to the number of contacts with physicians, including both generalists and specialists. There are variations across countries in the coverage of these consultations, notably in outpatient departments of hospitals. The data come mainly from administrative sources, although in some countries (Ireland, Italy, Netherlands, New Zealand, Spain and Switzerland) the data come from health interview surveys. Estimates from administrative sources tend to be higher than those from surveys because of problems with recall and non-response rates.
In Hungary, the figures include consultations for diagnostic exams such as CT and MRI scans (resulting in an over-estimation). The figures for the Netherlands exclude contacts for maternal and child care. The data for Portugal exclude visits to private practitioners (resulting in an under estimation). In Germany, the data include only the number of cases of physicians’ treatment according to reimbursement regulations under the Social Health Insurance Scheme (a case only counts the first contact over a three-month period, even if the patient consults a doctor more often, leading to an under-estimation). Telephone contacts are included in a few countries (e.g. Spain). In Turkey, a majority of consultations with doctors occur in outpatient departments in hospitals.
References
Delamaire, M.-L. and G. Lafortune (2010), “Nurses in Advanced Roles: A Description and Evaluation of Experiences in 12 Developed Countries”, OECD Health Working Paper, No. 54, OECD Publishing, Paris, https://doi.org/10.1787/5kmbrcfms5g7-en.
Devaux, M. and M. de Looper (2012), “Income-related Inequalities in Health Service Utilisation in 19 OECD Countries”, OECD Health Working Papers, No. 58, OECD Publishing, Paris, https://doi.org/10.1787/5k95xd6stnxt-en.
